FHIR-native EHRs improve interoperability, speed workflows, cut costs, and enable real-time alerts and AI-driven care.
FHIR-native EHRs are reshaping healthcare by addressing inefficiencies in outdated systems. Built entirely on the FHIR standard, these systems improve data sharing, streamline workflows, and enhance patient care. Here’s what they offer:
With 92% of EHR vendors now supporting FHIR APIs, clinics using these systems benefit from faster operations, reduced costs, and improved care. Delaying adoption risks falling behind on compliance and efficiency.
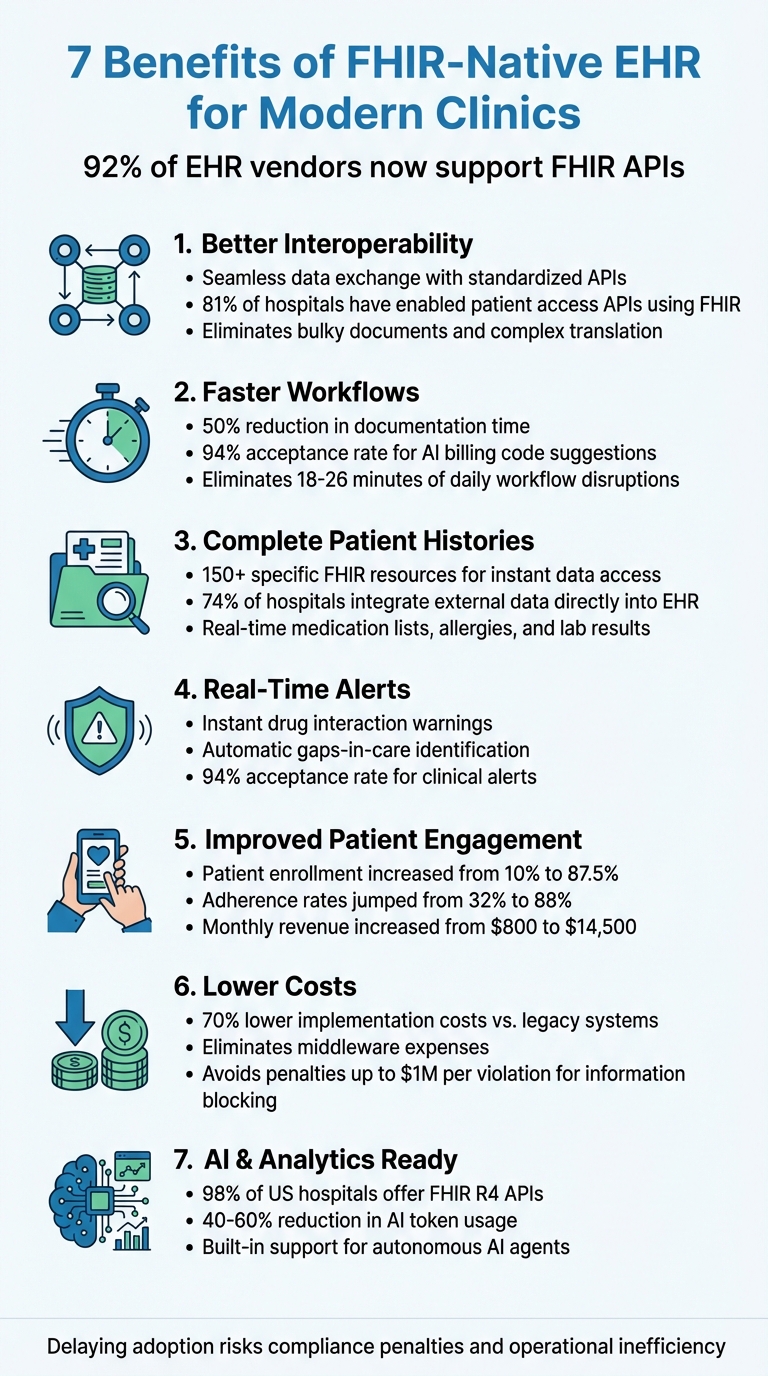
7 Key Benefits of FHIR-Native EHR Systems for Modern Clinics
FHIR-native systems are transforming how data is exchanged in healthcare. Unlike older systems that require retrofitted solutions, these systems allow direct, resource-specific API queries. For instance, clinics can instantly pull up a patient's medication list or recent lab results without needing to sift through bulky documents or rely on complex translation processes.
Another key advantage is semantic consistency. FHIR-native systems come with built-in terminology services that ensure standardized clinical codes like SNOMED CT, LOINC, and RxNorm retain their meaning across different platforms. This reduces data discrepancies and improves overall quality. By 2026, 92% of EHR vendors and 90% of health systems will support FHIR-enabled APIs, making seamless data sharing a reality.
These systems also bring noticeable improvements to clinical workflows. Take, for example, a U.S.-based health tech company that, in February 2026, switched from a legacy system to a FHIR-native, microservices-based EHR developed by Nirmitee. This transition, completed in just eight months by a team of six engineers, now supports three clinic locations and 45 providers.
With real-time data access, clinics save hours previously spent on manual tasks like faxing record requests or verifying medications over the phone. Instead, standardized APIs enable instant data sharing, allowing tools to automatically flag critical issues, such as drug–drug interactions - essential for urgent care scenarios.
One multi-location clinic with 120 providers saw dramatic results after adopting a native Epic RTM module. Patient enrollment jumped from 10% (120 patients) to 87.5% (1,050 patients), while monthly revenue soared from $800 to $14,500. These gains were achieved by eliminating 18–26 minutes of daily workflow disruptions.
"The true adoption limiter is workflow integration. When RTM requires staff to work 'outside' their existing EHR environment, adoption collapses regardless of clinical benefit." - clinIQ Healthcare
Beyond workflow efficiency, this architecture also supports scalability and reduces costs.
FHIR-native systems are cost-effective in the long run, as they eliminate the need for custom HL7v2 interfaces. Unlike HL7v2, which requires tailored connections for every data source, FHIR uses standardized APIs that can link to multiple endpoints. This makes it easier and cheaper for clinics to integrate new data sources as they expand.
Regulations also play a role in driving this shift. Starting in September 2025, penalties for information blocking can reach up to $1 million per violation, pushing clinics toward electronic data sharing. FHIR-native systems help clinics comply with these rules effortlessly. Currently, 81% of non-federal acute care hospitals have already enabled patient access APIs using FHIR, solidifying its place as the modern standard for healthcare data exchange.
FHIR-native systems are transforming daily healthcare operations by simplifying and speeding up processes. Tasks like faxing record requests or manually entering patient data are replaced with instant data transfers. Information such as medications, allergies, and lab results is shared seamlessly between systems using discrete codes, cutting out the need for time-consuming phone calls or retyping details from scanned documents.
Smart templates and tools like SNOMED CT autocomplete streamline documentation by pre-filling clinical notes based on the visit type. On top of that, AI-powered billing code suggestions save time by reducing the need for manual coding. These enhancements lead to faster, more accurate documentation, improving overall clinic efficiency.
Another major benefit is the elimination of "app switching." Logging into separate platforms for tasks like Remote Therapeutic Monitoring (RTM) can disrupt workflows, adding 18–26 minutes of extra effort. With native integration, this disruption drops to 14–20 minutes, as staff can manage everything within a single platform.
"Workflow disruption creates cognitive burden. Even 5–10 minutes of daily 'tool switching' compounds to 40–80 hours per provider annually - equivalent to eliminating 1–2 weeks of clinical capacity per provider." - clinIQ Healthcare
AI-driven tools further cut down on manual work. Features like ambient scribes and history chatbots automatically draft notes and document patient histories. Meanwhile, AI assistants suggest CPT and ICD-10 codes based on encounter details, making coding faster and more accurate. Currently, 74% of hospitals directly integrate external data into their EHR systems, moving beyond basic viewing to automated workflows. These advancements are setting the stage for even more efficient, AI-enhanced clinic operations.
FHIR-native EHRs store patient data in the FHIR R4 format, which eliminates delays caused by data translation or mapping errors. Imagine a patient arriving at your clinic after seeing another provider - you can immediately access their medication lists, allergy history, lab results, and problem lists.
With patient records divided into over 150 specific resources (like MedicationRequest, Observation, and Condition), clinicians can quickly query the exact information they need in real time. No more digging through lengthy documents. This standardized approach ensures seamless connections between your clinic, labs, pharmacies, and other health systems.
Having access to complete patient histories significantly reduces the time spent on documentation. External data, such as a patient’s medication history from another provider, is automatically imported into their chart as coded entries. This means medication lists populate instantly - no need for manual data entry from scanned documents.
"Urgent care centers can check what antibiotics a patient received last week before prescribing more. Telehealth platforms can access the same comprehensive patient view that in-person clinicians see."
– Maxim Rotaru, Founder & CEO, Webamboos
Instead of juggling multiple platforms or piecing together fragmented records, everything clinicians need is available in one place. Currently, 74% of hospitals integrate external data directly into their EHR systems rather than viewing it on separate platforms. This eliminates the need for tool switching, which can add 18–26 minutes to workflows. With instant access to accurate data, clinicians can document faster and make well-informed decisions more quickly.
Beyond efficiency, having complete patient histories improves patient engagement and care quality. Providers in urgent care settings, for example, can make real-time decisions by instantly verifying recent prescriptions, flagging potential drug interactions, and reviewing allergy details - even for first-time or unconscious patients. Longitudinal views of lab results also help uncover trends that might not be obvious during a single visit.
An example of this in action is Ottehr, an AI-driven, FHIR-compliant EHR tailored for urgent care. As of April 2026, it has supported over one million urgent care visits. The platform incorporates tools like SMS-based patient engagement and AI-powered medical history chatbots directly into clinical workflows, reducing charting time while improving overall care. Patients also gain better transparency through SMART on FHIR apps, which allow them to track progress and follow-up instructions using data pulled directly from the clinic’s system.
FHIR-native EHRs take clinical decision-making to the next level with real-time alerts that kick in during documentation. Imagine this: as a clinician prescribes a medication, the system instantly scans for drug-drug interactions or duplicate prescriptions from the past week. No need for time-consuming manual checks. This automatic alerting system blends seamlessly into workflows, eliminating delays and boosting efficiency.
Take a real-world example: in February 2026, a US-based health tech company teamed up with Nirmitee.io to develop a FHIR-native EHR for three clinics serving over 12,000 patients. In just eight months, a six-person engineering team delivered a system that cut documentation times by 50%. It included real-time clinical decision support to block critical drug interactions and flag abnormal lab results. Providers received auto-notifications with a 94% acceptance rate for billing code suggestions.
"Clinical decision support: real-time alerts as the provider documents - drug interactions, preventive care reminders, clinical guideline suggestions."
– Nirmitee.io
Thanks to FHIR's granular resources like MedicationRequest and Observation, these systems can process urgent queries instantly - no complicated data transformations required. This means critical lab values can be flagged in real-time, enabling providers to act immediately. Dashboards refresh on the fly, ensuring clinicians always have the latest data at their fingertips.
Real-time alerts aren't just about efficiency - they also tackle gaps in preventive care. These systems can identify missing immunizations, overdue screenings, or concerning lab trends using visual tools like "sparklines". Instead of waiting for a follow-up visit or a quality audit, providers can address these issues right then and there, while the patient is still in the room.
FHIR's use of standardized vocabularies like SNOMED CT, LOINC, and RxNorm ensures that data from external systems - whether it's a diagnosis, lab result, or prescription - is interpreted correctly to trigger relevant alerts. With 90% of health systems using FHIR-enabled APIs by 2026, clinics can now pull real-time data from external pharmacies, labs, and other providers. This broader data access allows clinicians to spot care gaps that might not appear in a local record, enabling informed decisions even for first-time patients.
FHIR-native EHRs make accessing health data as simple as checking your bank balance on a mobile app. Thanks to widespread adoption, patients can now effortlessly access, download, and share their medical records. A unified patient portal brings together lab results and records from across the country, allowing seamless record sharing through TEFCA's Individual Access Services.
"Practices that make this easy earn loyalty. Practices that make it hard lose patients" – EHRSource
This level of streamlined data access not only puts patients in control of their health information but also sets the stage for better care outcomes.
Beyond easy access to data, FHIR-native systems come equipped with tools that drive patient engagement and improve care quality. For example, a multi-location clinic saw patient enrollment jump from 35–40% to 87.5%, while adherence rates soared from 32% to 88%. This switch to a native RTM module generated a net benefit of $65,550 in just six months.
One major challenge in standalone monitoring programs is patient friction, which accounts for 40% of dropouts. Patients often forget to use separate apps, get confused about their status, or abandon the process when faced with multiple logins. Native integration eliminates these hurdles by embedding monitoring tools directly into the EHR interface patients already use for scheduling, messaging, and viewing results. Features like built-in scheduling, telehealth, and SMS messaging create a smooth experience from the first appointment to follow-up care.
Additionally, AI-driven chatbots within FHIR-native systems simplify patient intake processes and cut down wait times. This allows clinicians to spend more time on face-to-face care, ultimately improving patient satisfaction and outcomes.
FHIR-native EHRs eliminate the need for middleware, which traditional systems rely on to convert proprietary data into shareable formats. By storing data directly in FHIR format, clinics avoid the recurring costs of transforming information every time they need to exchange it with labs, clearinghouses, or patient apps.
This approach leads to immediate savings. A February 2026 case study revealed that implementation costs for FHIR-native systems were about 70% lower than legacy solutions. Clinics also benefited from faster performance, with page loads under 800ms, making operations smoother and growth more manageable.
The microservices architecture of FHIR-native systems adds another layer of flexibility. Clinics can scale individual modules - like scheduling or billing - without having to overhaul their entire infrastructure. Plus, cloud-native deployment simplifies the process of adding new locations by removing the need for manual firewall configurations or VPN setups.
Compliance becomes more straightforward and cost-effective as well. With built-in FHIR support, clinics can meet the requirements of the 21st Century Cures Act without additional development, avoiding penalties that can go up to $1 million per violation for information blocking.
For smaller practices, platforms like Ottehr Clinical make advanced FHIR-native technology accessible, starting at $349 per provider per month. This includes features like AI scribe, ePrescriptions, and custom branding, offering a comprehensive solution at an affordable price.
These advantages not only reduce costs but also prepare clinics to adopt new technologies that can improve patient care and operational efficiency.
FHIR-native systems are opening doors to advanced AI and analytics capabilities, thanks to improvements in interoperability and streamlined workflows.
FHIR-native EHRs store data in standardized formats like Patient, Observation, and MedicationRequest resources right from the start. This eliminates the need for complex data transformations when integrating with AI tools. Essentially, FHIR now acts as the "operating system" for AI agents.
With 98% of US hospitals now offering FHIR R4 APIs, clinics have a ready-to-use data layer for AI integration. Using established clinical standards like LOINC for labs, SNOMED CT for findings, and RxNorm for medications, AI models can directly interpret structured data without the need to sift through unstructured text. Through standard REST API calls, AI agents can both read clinical histories and write results back into the EHR.
FHIR-native systems enable real-time AI integration with tools like CDS Hooks, which can trigger alerts in under 500ms during tasks like order entry or chart reviews. The Model Context Protocol (MCP-FHIR) provides a structured way for large language models to interact with FHIR APIs, allowing them to read or write clinical data efficiently.
These systems have already shown measurable benefits. For example, AI-powered smart templates and autocomplete features have cut documentation time by 50%, while AI-suggested billing codes boast a 94% acceptance rate. Additionally, by selectively loading FHIR resources, large language models can reduce token usage by 40–60%, making AI processes more efficient.
By seamlessly integrating AI, FHIR-native systems improve both patient care and clinician support. Modern systems now enable "Agentic AI", where autonomous agents can identify risks, draft care plans, and suggest orders for clinician review. These agents write to the EHR with statuses like status: draft and intent: proposal, ensuring clinicians retain full control.
To ensure transparency and regulatory compliance, the emerging HL7 AI Transparency specification embeds metadata like model versions, confidence scores, and evidence links directly into FHIR resources. This makes AI-influenced decisions traceable and auditable.
Platforms such as Ottehr Clinical make these advanced tools accessible, offering plans at $349 per provider per month. Features include an AI coding assistant and diagnostic order capabilities integrated with core clinical functions. For smaller clinics, the free Ottehr AI tier provides tools like an HPI chatbot and ambient scribe, making AI-powered documentation accessible to all.
FHIR-native EHR systems are changing how clinics handle patient data, streamline workflows, and deliver care. By using standardized FHIR R4 formats from the beginning, these platforms sidestep the challenges of outdated systems. The payoff? Quicker workflows, effortless data sharing, and improved patient care - all while easing the administrative load on healthcare providers.
The numbers paint a clear picture: 92% of EHR vendors now support FHIR R4, and 90% of health systems use FHIR-enabled APIs. The industry has reached a critical point where staying with older systems could mean falling behind. Clinics that delay transitioning risk hefty penalties for information blocking - up to $1 million per violation. Beyond compliance, the switch to FHIR-native systems offers tangible efficiency gains.
For clinics looking to make the leap, platforms like Ottehr provide an accessible starting point. Their free tier includes AI-powered tools like ambient scribes and HPI chatbots. As needs expand, clinics can upgrade to the Clinical plan at $349 per provider per month, unlocking features like ePrescriptions, lab integrations, and AI coding assistants. This step not only boosts efficiency but also sets clinics up for sustainable growth.
A FHIR-native EHR is designed from the ground up using FHIR (Fast Healthcare Interoperability Resources) principles. It leverages FHIR APIs and data models as its core framework, enabling smooth, real-time data exchange without needing extra transformation layers.
On the other hand, FHIR-enabled systems only support FHIR standards but often depend on additional middleware to achieve interoperability. This distinction makes FHIR-native solutions not only more efficient but also better suited to meet regulatory requirements like the 21st Century Cures Act.
Migrating to a FHIR-native EHR system comes with its fair share of challenges, primarily due to technical complexities and compliance requirements. The process involves converting data from proprietary formats into FHIR standards, which demands meticulous attention to ensure data integrity. Additionally, handling large volumes of sensitive patient information adds another layer of responsibility.
Integrating with modern FHIR APIs isn't straightforward either. It often requires detailed mapping of data fields, rigorous testing, and thorough validation to ensure everything functions as expected. To navigate these hurdles effectively, a well-thought-out plan and a phased implementation approach are essential. This helps minimize disruptions to operations and ensures the accuracy of data throughout the transition.
FHIR-native EHRs prioritize patient data security when sharing information via APIs. They achieve this through features like fine-grained access control, role-based permissions, and encryption. By enforcing a 'need-to-know' approach, these systems ensure that only authorized individuals can access specific portions of data. At the same time, they adhere to strict security regulations to maintain compliance and protect sensitive information.